
How can educators promote resilience in students who have experienced trauma?
In the late 1990s, medical researchers began to study the effects of Adverse Childhood Experiences, or ACEs, on children’s long-term health and wellbeing. [i]
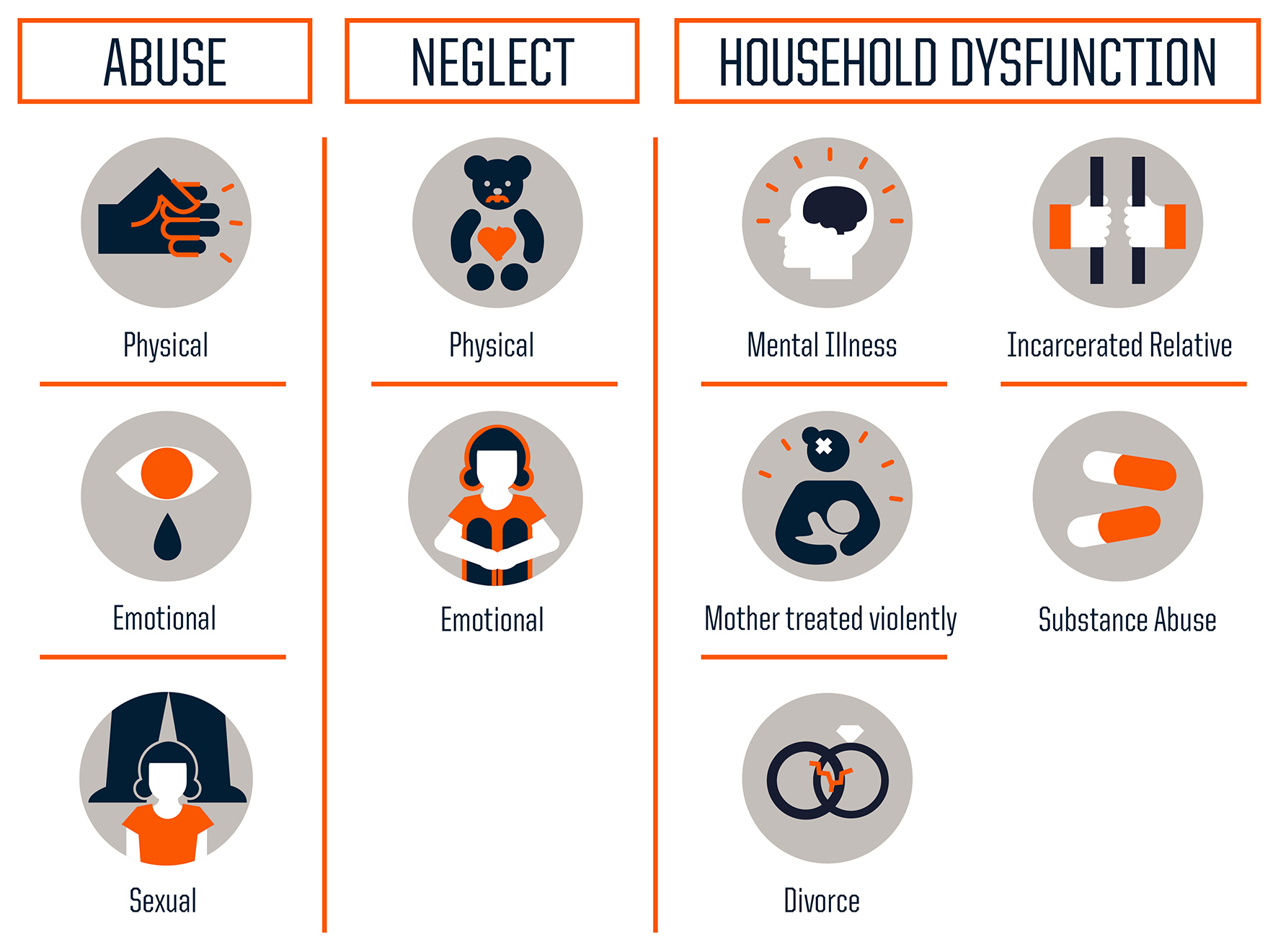
Three types of adversity that make for a tough childhood.
ACES include severe, frequent stressors or traumatic situations, such as abuse, neglect, and household dysfunction. [ii, iii, iv] When individuals lack supportive relationships or resources to cope with these stressors, their bodies’ stress response is over-activated, resulting in harm to their physical, social, emotional, and cognitive well-being. [ii, iv] This is known as a toxic stress response to trauma. [ii]
Now education researchers are studying how trauma exposure affects students’ ability to learn, and how schools can support these students. [i] This emerging research is relevant for all educators, as studies suggest at least 38 percent of children in every state have had at least one ACE. [iv] Children who belong to historically marginalized racial/ethnic groups experience ACEs at higher rates [v], as well as those from low-income families [iv]; however, ACES impact children across all races/ethnicities and levels of income. [iv]
In the Key Findings, we share research on how trauma affects student development and learning, and ways to help students experiencing trauma to become more resilient.

Without intervention, toxic stress can alter a child’s brain structure, causing numerous long-term health issues.
[vi] Some are physical, such as increased rates of obesity and chronic illness, while others are emotional and social, such as increased rates of depression and anxiety, difficulty controlling emotions, and challenges forming healthy relationships. [vi, vii, viii] Trauma exposure can also lead to deficits in memory and impulse control [ix], and difficulties with executive functions such as planning, organizing, and synthesizing information. [vii]
Trauma is most damaging when it occurs regularly over time, and some studies indicate that children who experience four or more ACEs are at the greatest risk for adverse consequences. [vi, x] However, even one-time traumatic experiences such as witnessing violence or the death of a loved one can lead to toxic stress if a child does not have supportive adults to buffer them from the effects of the trauma. [ix] Further, the consequences are most detrimental for children who experience toxic stress early in life (ages 0-5) when the brain is developing rapidly. [ix, xi]
Individuals who experience trauma often have deficits in executive function and self-regulation of behavior and emotions, both of which play a significant role in learning. [v, vii, xii] Further, research points to a link between trauma and difficulties developing language and reading skills. [i, vii]
In school, students who have experienced trauma may have trouble calming down, may become easily distracted or be disengaged, and often find it hard to make friends. [iv] Educators might also notice these students are easily aroused or have intense emotions, and have low self-esteem and either under- or over-controlled behaviors. [xiii] Further, students may have low trust in authority, and irregular attendance. [i]
Fortunately, the human brain has the potential to grow and change throughout the lifespan. [ix] The following research-based interventions can help improve health and learning outcomes for students who have experienced trauma.
High-quality early education programs can improve young children’s outcomes by boosting their learning skills and connections to responsive, caring adults. [v, xiv] Further, screening — in medical offices, schools, and other community sites — can identify children experiencing toxic stress and provide support to stem its negative effects. [ii, vii]
It is also helpful to build caregivers’ skills so they can better support children experiencing trauma. For example, research points to coaching caregivers in responsive “serve and return” interactions, where an adult responds to a young child’s sounds or gestures with eye contact, words, or touch. [xv] This strengthens the bond between the caregiver and child, and helps improve the child’s communication and social skills. Further, caregivers need to receive treatment for any health issues they experience as a result of trauma, so they can help prevent their child’s exposure to traumatic situations and teach them healthy ways to regulate emotions. [v, viii, xiv]
 Youth of all ages can learn to become more resilient in the face of stressors, meaning they can develop skills to respond to challenges in a healthy and flexible way. This is important, as resilience can help minimize the negative outcomes of trauma. [v, xiv] One approach to improve this skill is to connect youth with a supportive adult who can shield them from stressors and coach them in managing emotions and behavior. [iv, xiv] It is also important to help students enhance their executive function skills through programs that invite them to practice focusing attention, solving problems, planning ahead, and adjusting to new circumstances. [vii, xiv]
Youth of all ages can learn to become more resilient in the face of stressors, meaning they can develop skills to respond to challenges in a healthy and flexible way. This is important, as resilience can help minimize the negative outcomes of trauma. [v, xiv] One approach to improve this skill is to connect youth with a supportive adult who can shield them from stressors and coach them in managing emotions and behavior. [iv, xiv] It is also important to help students enhance their executive function skills through programs that invite them to practice focusing attention, solving problems, planning ahead, and adjusting to new circumstances. [vii, xiv]
A specific strategy is to guide students as they practice coping with “manageable stress” (such as giving a speech in front of the class) so they are prepared for more severe stressors. This practice is useful for all youth, not just those who have previously experienced trauma. [xiv]
Schools can play a vital role in supporting youth who have experienced trauma. Staff can conduct trauma screening, and then connect students to mental health services on- or off-site. [i, ii, xvi] They can also work with families and local partners to make communities safer, and offer resources to support students’ caregivers. [iv, xi, xiv] Further, school staff benefit from training on trauma’s effects and ways to respond to students’ social, emotional, behavior, and learning difficulties. [i, xiii, xvi]
Schools can also consider using trauma-informed behavior management strategies, which avoid punitive or exclusionary discipline practices that can re-traumatize students or reinforce their sense of alienation and lack of trust in authority. [i, xiii, xvi] There is some evidence to support the Positive Behavior Intervention (PBI) approach, in which staff communicate clear expectations for all students and focus on behaviors they want to see vs. those they want to eliminate. [xiii] Educators are encouraged to be mindful of students’ challenges by asking, “What happened to you?” rather than “What’s wrong with you?” when they encounter challenging student behaviors. [i]
Citations
[i] McInerney, M. and McKlindon, A. 2014.Unlocking the Door to Learning: Trauma-Informed Classrooms & Transformational Schools.” Education Law Center.
[ii] Harris, N.B., Marques, S.S., Oh,, D, Bucci, M., and Cloutier, M. 2017. “Prevent, Screen, Heal: Collective Action to Fight the Toxic Effects of Early Life Adversity.” Academic Pediatrics: 17(S14–S15).
[iii] National Survey of Children’s Health. Child and Adolescent Health Measurement Initiative. Data Resource Center for Child and Adolescent Health. 2016 National Survey of Children’s Health (NSCH) data query. Retrieved [04/29/18] from www.childhealthdata.org. CAHMI: www.cahmi.org.
[iv] Robert Wood Johnson Foundation. 2017. “Traumatic Experiences Widespread Among U.S. Youth, New Data Show.” Retrieved [04/29/18] from https://www.rwjf.org/en/library/articles-and-news/2017/10/traumatic-experiences-widespread-among-u-s–youth–new-data-show.html. CAHMI: www.cahmi.org.
[v] Cantor, P, Osher, D., Berg, J., Steyer, L. and Rose, T. 2018. Malleability, plasticity, and individuality: How children learn and develop in context, Applied Developmental Science, DOI: 10.1080/10888691.2017.1398649.
[vi] Anda, R.F, Felitti, V.J., Bremner, D., Walker, J.D., Whitfield, C., Perry, B.D., Dube, S.R., and Giles, W.H. 2006. “The enduring effects of abuse and related adverse experiences in childhood: A convergence of evidence from neurobiology and epidemiology.” European Archives of Psychiatry and Clinical Neuroscience 256(3): 174–186. doi:10.1007/s00406-005-0624-4.
[vii] Perkins, S. and & Graham-Bermann, S. 2012. “Violence Exposure and the Development of School-Related Functioning: Mental Health, Neurocognition, and Learning.” Aggression and Violent Behavior 17(1): 89–98. doi:10.1016/j.avb.2011.10.001.
[viii] Kim, J. and Cicchetti, D. 2010. “Longitudinal pathways linking child maltreatment, emotion regulation, peer relations, and psychopathology.” Journal of Child Psychology and Psychiatry 51(6): 706–716. doi:10.1111/j.1469-7610.2009.02202.x.
[ix] Center for Youth Wellness. 2014. “An Unhealthy Dose of Stress: The Impact of Adverse Childhood Experiences and Toxic Stress on Childhood Health and Development.”
[x] Sacks, V., Murphey, D., and Moore, K. 2014. “Adverse Childhood Experiences: National and State-Level Prevalence.” Child Trends.
[xi] Davis, M., Costigan, T., and Schubert, K. 2016. “Promoting Lifelong Health and Well-being: Staying the Course to Promote Health and Prevent the Effects of Adverse Childhood and Community Experiences.” Robert Wood Johnson Foundation 17(7): S4-S6. DOI: 10.1016/j.acap.2016.12.002
[xii] DePrincea, A.P., Weinzierl, A., Melody, D., and Combs, B. 2009. “Executive Function Performance and Trauma Exposure in a Community Sample of Children.” Child Abuse & Neglect 33(6):353-61.
[xiii] Keels, M., Staff, J. and Griffin, R. 2017. “Trauma Responsive Education Practices: A Conceptual Framework.” Practice Brief #1. TREP Project.
[xiv] National Scientific Council on the Developing Child. (2015). “Supportive Relationships and Active Skill-Building Strengthen the Foundations of Resilience: Working Paper 13.”
[xv] Harvard University Center on the Developing Child. (n.d.) “Serve and Return.”
[xvi] Pickens, I.B. and Tschopp, N. (2017). “Trauma-Informed Classrooms.” National Council of Juvenile and Family Court Judges.